
For individuals living with Sickle Cell Disease (SCD), knowing as much as possible about the disease will help you to better manage and reduce complications.
The Sickle Cell Awareness Group of Ontario (SCAGO) works closely with health care professionals and the Ontario Ministry of Health and Long Term Care to ensure that individuals living with SCD receive the best care possible.
What is Sickle Cell Disease?
Red blood cells contain a protein called Hemoglobin. This protein carries oxygen around the body and keeps your vital organs working. Normal Hemoglobin is called Hemoglobin A (HbA), but you can also inherit different types of hemoglobin from your parents.
Sickle Cell Disease (sometimes also called Sickle Cell Anemia) is a condition you are born with. It is caused by an abnormal form of hemoglobin.
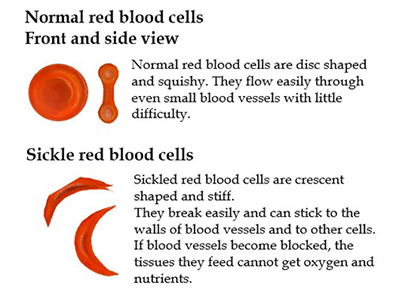
With SCD, the abnormal hemoglobin, known as hemoglobin S (HbS), has a tendency to crystallize inside the red blood cell and become rigid, especially when it is not carrying any oxygen molecules.
Because of this crystallization, the red blood cell becomes stiff, brittle and sticky. It is easy therefore for red blood cell to breakdown (this is commonly called hemolysis) and to block up and damage blood vessels.
Because of hemolysis people with SCD have anemia or weak blood. Other problems arise when blood vessels get blocked and tissues do not get the oxygen they need. This causes tissue injury often resulting in pain. Recurrent injury to organs can cause permanent damage.
What are the Complications to Look for?
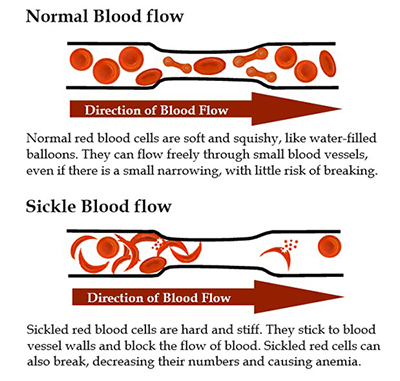
SCD causes problems in two ways: By breakdown of the red blood cell (hemolysis) and by blocking the flow of blood in the blood vessels (vaso-occlusion).
The most common symptom is pain, especially in the bones. Other complications include damage to shoulder and hip joints (avascular necrosis), chest pain with difficulty breathing (acute chest syndrome) and priapism.
There are also many problems, which may not cause symptoms at first. These include damage to the lungs and heart (which may lead to pulmonary hyper-tension, which can cause heart failure), as well as damage to the kidneys, liver and eyes. Other problems include stroke and leg ulcers.
SCD patients are also at increased risk from infections, particularly during childhood. Because it can damage all of these body “systems”, SCD is an example of a “multisystem disorder”.
 How can I Avoid Developing These Complications?
How can I Avoid Developing These Complications?
Many complications can be prevented or reduced by adhering to your care provider’s prescribed treatment. This may include preventative strategies such as regular blood tests and diagnostic imaging studies, medications such as hydroxyurea, and the use of blood transfusions.
There are also simple lifestyle changes that can make a big difference.
These include:
- Avoid dehydration – drink a lot of fluids.
- Get regular exercise.
- Eat a good diet with lots of fruits and
- Don’t smoke or use recreational drugs.
- Find ways to reduce the amount of stress in your life – consider yoga, mindfulness, or meditation.
- Avoid extreme temperatures; check the weather before you go out and always be prepared for it.
- Make sure you are up to date with recommended vaccinations.
- Remember you are not Reach out to family, friends and members of your community and support groups like SCAGO.
By seeing your doctor in clinic when you are feeling well and not in crisis, you have an opportunity to discuss these important ways of coping with SCD, which may help to reduce complications.
How do I Manage the Pain (crisis) that Affects my Chest, Legs, and Arms from Time to Time?
The best way to treat pain crises is to try and prevent them in the first place by sticking to the lifestyle changes we just spoke about. You should also follow your doctor’s treatment recommendations, such as using your hydroxyurea.
If you feel a crisis coming on, try to rest and drink plenty of fluids and use your pain killers/analgesia. It is easier to stop a pain crisis getting worse if you hit the pain hard when it first comes on.
When Should I go to the ED?
- Medical assistance should be sought if the pain is accompanied by a fever, difficulty breathing, or confusion.
- If you cannot bring the pain under control without experiencing significant side effects from your pain medications or
- If you are unable to maintain adequate fluid intake due to stomach pain or nausea.
- If you are experiencing Priapism, a painful crisis affecting the penis, resulting in a prolonged and painful erection in the absence of sexual It may come and go over short- periods (stuttering priapism), but if it lasts for more than two hours, medical attention should be sought in order to avoid permanent damage.
If you are experiencing chronic pain, this may indicate a structural problem, such as avascular necrosis (damage to you shoulder or hip joint), or damage to the nerves themselves. Treating chronic pain is a long-term process that often requires specialty care not available in an emergency department. Chronic pain does not respond well to analgesics commonly used in Sickle Cell Disease. Seeing a pain specialist may help.
Treatment Options
What is Hydroxyurea?
Hydroxyurea is a drug (capsule) originally used to treat some forms of blood cancer (Leukemia) and blood disorders that can later turn into Leukemia. It has been used for over 30 years
to treat SCD and has been shown to be extremely safe. There is no evidence that it can cause cancer and good evidence that it can increase life expectancy.
Hydroxyurea works in a few different ways, but its main mechanism is to increase your body’s production of fetal (baby) hemoglobin ( HbF) instead of the adult hemoglobin, which contains the sickle mutation.
Like all drugs, it does have some side effects, and therefore requires regular blood test monitoring. Also, unlike pain killers which you take when required, hydroxyurea must be taken every day to be effective.
Hydroxyurea is the only drug therapy available for SCD and has been shown to prolong survival, reduce pain episodes and reduce some of the complications.
What is the Difference Between Blood Transfusion and Blood Exchange Therapy?
Blood transfusions in SCD can be carried out in 1 of 3 ways.
The easiest way is to simply transfuse units of blood. This is also known as a “top-up transfusion”. This improves the supply of oxygen to your body but also makes your blood thicker and less able to flow through small blood vessels. As a result, top-up transfusions are usually only performed if you are extremely anemic.
Otherwise, the preferred means of blood transfusion is to remove some of your own blood first, and then transfuse. This can be done manually (similar to giving a blood donation followed by receiving a transfusion) or through a special procedure known as erythrocytopheresis.
This involves hooking you up to a machine that automatically replaces your blood in small volumes, multiple times, until only a very small amount of sickle hemoglobin remains in circulation.
When do I Need Blood Transfusion and/or Blood Exchange Therapy?
Transfusions are most commonly given for patients who have had a stroke or are found to be at high risk of having a stroke, or for those scheduled for surgical procedures. It can also be given in the setting of acute organ failure, such as an acute chest syndrome. In rare circumstances it may be required during pregnancy or to treat very severe anemia (e.g. hemoglobin less than 50 g/L).
However, transfusions can also cause harm if given in the wrong setting (e.g. for the treatment of uncomplicated pain crisis). For this reason, it is recommended that transfusions for patients with sickle cell disease only be ordered by blood specialists (hematologists).
Is There a Cure for Sickle Cell Anemia?
At present, there is only one cure for SCD – bone marrow or stem cell transplantation. This is a potentially dangerous procedure that requires identifying a well-matched donor, and is usually only performed in children. There is a great deal of progress being made in gene therapy, however, and if successful this will allow for cure in a much larger number of patients than are currently offered bone marrow or stem cell transplantation.
Good to Know! – Important Facts about Blood Transfusions
 Why is phenotype-matched blood better for me?
Why is phenotype-matched blood better for me?
Phenotype-matched blood means that the blood has been matched to you much more carefully than is regularly performed. This reduces the chance of having a transfusion reaction and of developing an antibody to the blood you are transfused. However, in Canada, because most blood donors are from ethnic backgrounds different than SCD patients, there is a limited supply of phenotypically- matched blood.
How can I help increase phenotype-matched blood reserve?
Canadian Blood Service (CBS) is looking for more blood donors from ethnic minorities. If you have friends or family who want to help people with SCD, becoming a blood donor is a very practical, valuable and worthwhile way to help. If you would like to arrange a blood donor drive or session in Ontario, SCAGO can help with this. Note that you cannot donate blood if you have SCD. However, individuals with sickle cell trait can still donate.

